 
It is important to begin moving as soon as possible. Most patients are able to get of bed and start physical therapy the day after surgery. 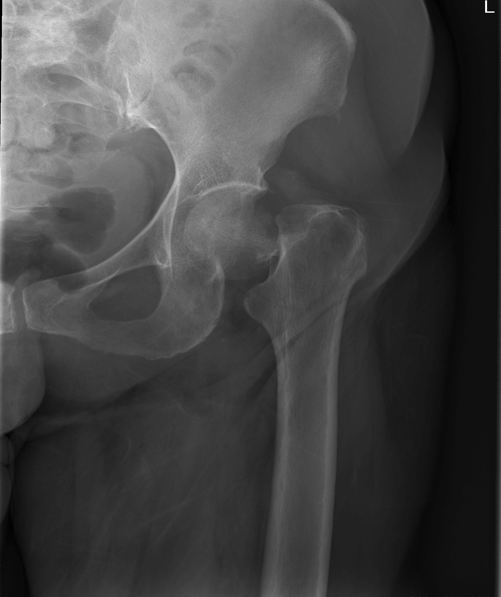
Pinning prevents the femoral head from dislodging or slipping off of the femoral neck, a situation that would require hip replacement. In this procedure, surgical pins or screws are passed across the fracture site to hold the ball of the femur in place while the fracture heals. If a femoral neck fracture is not displaced, the most common treatment is in-situ pinning. This type of fracture is also sometimes called a subcapital or intracapsular fracture. Treatment for a hip fracture depends upon the type and location of the fracture, as well as the age and condition of the patient. Even if it does takes longer, it is better to be optimized than to rush to surgery. Ideally, it should be done within 48 hours, but sometimes it may take longer. This process of getting a patient medically ready for surgery is called optimization. If you have been on a blood thinner, you may need to wait for your clotting times to improve before you go to the operating room. In some cases, you may need to be seen by a specialist, such as a heart doctor (cardiologist) or a lung doctor (pulmonologist), to treat specific medical problems. They will make sure that you are medically ready to have surgery. If you are admitted to the hospital with a hip fracture, you will have preoperative testing and will most likely be seen by an internist. Having surgery as soon as possible can lessen the risk of complications. Surgical treatment is required to relieve the acute pain of the fracture and to allow the patient to get out of bed. Only a very small group of nondisplaced fractures in healthy patients can be treated without surgery, while a separate small group of patients may be too sick to safely have surgery. Most hip fractures require surgical treatment within 1 to 2 days of injury. Most hip fractures can be diagnosed with an X-ray. X-rays provided images of dense structures, such as bone. Imaging studies will help confirm the diagnosis and provide more information about the fracture. With this type of fracture, you may still be able to move your leg and bear weight even though it is painful. In this situation, you may choose to go to a doctor’s office rather than an emergency room. Typically, these are nondisplaced fractures of the femoral neck. There may be a bruise on the outer part of the hip or thigh at the point of impact where you fell, and all movement will be limited and painful.Ī small number of hip fractures may not be as painful at first. Often, the injured leg will appear shorter than the opposite leg and will be twisted or rotated, either internally or externally. The doctor will also check the sensation, movement, and circulation in your lower leg. 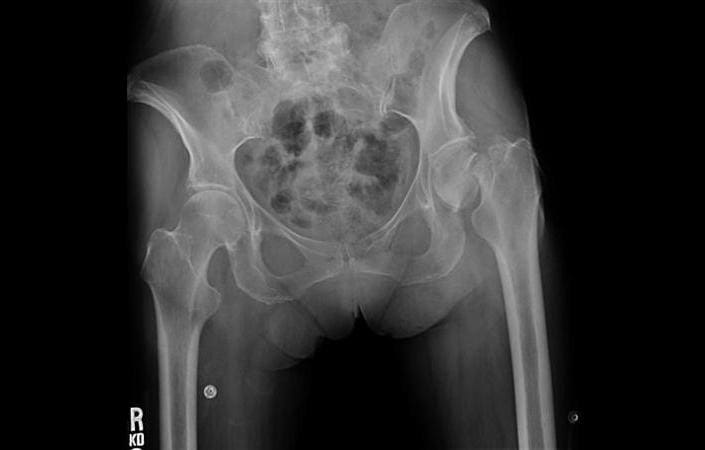
They will take a history of your injury and check to make sure that you do not have injuries to other parts of your body. DAA requires an experienced surgeon and careful patient selection.Most of the time, a patient with a hip fracture will be taken by ambulance to a hospital emergency room.Īt the hospital, you will be examined by either an emergency room physician or an orthopaedic surgeon. It could lead to more intraoperative complications and a higher revision rate. Results suggest that DAA does not provide any early functional benefit in THA-DMC for FNF compared to PLA. Cup anteversion was 6° greater and inclination 9° lesser in DAA group (p=0.028, p<0.01). There were 3 revisions in the DAA group (1 infection, 1 dislocation, 1 peri prosthetic fracture) and 1 in the PLA group (infection), which was not statistically significant (p=0.34). DAA was associated with more intraoperative complications with 4 fractures and 1 femoral nerve deficit (p=0.018). There was no significant difference in HHS or Parker score at 3 and 12 months follow up (p=0.6, p= 0.75). Radiographic data of cup positioning and limb length were evaluated.įifty-two patients were included in the DAA group and 54 in the PLA group. One year clinical results and all cause revision rate were also collected. Intraoperative complications were collected during hospitalization. The primary endpoint was Harris Hip Score and Parker score assessed at the first follow-up visit. The aim of this study was to compare the early functional results of DMC in FNF by DAA versus posterolateral approach (PLA).Ī prospective study was conducted on a continuous series of patients who received DMC for FNF by DAA or PLA. Direct anterior approach (DAA), historically promoted for better stability, has been developed in recent years for better functional results. Dual mobility cups (DMC) reduce the risk of dislocation in femoral neck fractures (FNF). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
